Comparison of open and laparoscopic inguinal hernia repair
Abstract
Inguinal hernia repair is one of the most commonly performed general surgery operations. Throughout the years there have been many variations and advancements, including open and laparoscopic techniques, to accomplish the same task of reducing herniated contents and preventing groin hernia recurrence. An array of factors contributes to deciding which operative technique is the best approach to managing a patient presenting with an inguinal hernia. Published data vary due to the heterogeneity of techniques compared, patient presentations, and surgeon expertise. In experienced hands, laparoscopic repair results in a quicker return to work and reduced postoperative pain. Patients with bilateral groin hernias, female patients with groin hernias, and patients with recurrent hernias after prior anterior mesh repair should be offered a laparoscopic preperitoneal mesh approach, when surgeons have the appropriate skill set and experience. We find that open and laparoscopic techniques of inguinal hernias can both achieve exceptional outcomes when applied to the right patient population. To know one’s own capabilities, it is beneficial for surgeons to have baseline familiarity of the multitude of methods of repair, become proficient in both mesh and mesh-free techniques as well as open and laparoscopic techniques to best tailor the surgery to the patient and the clinical circumstances, and follow personal outcomes to evaluate individual results.
Keywords
Inguinal hernia repair is one of the most common operations in general surgery, with over 700,000 inguinal hernias repaired in the United States annually[1,2,3]. Throughout the years there have been many advancements in the operation including the genesis of laparoscopic techniques. With a multitude of surgical methods, it can often become difficult in deciding the best method of repair. An array of factors contributes to deciding which operative technique is best utilized for a patient presenting with an inguinal hernia. We will explore these variables as well as the surgical techniques themselves.
SURGICAL TECHNIQUES
Open inguinal hernia repairs can be categorized into two main categories: tissue repair and mesh repair [Table 1]. There are several named techniques that can be utilized for performing a tissue repair such as the Bassini, McVay, Marcy, and Shouldice repairs[4,5,6]. The Desarda repair, a more recently described tissue repair, utilizes a partially detached strip of external oblique aponeurosis[7]. For open mesh repairs, prosthetics are either placed anteriorly or preperitoneal. The gold standard mesh repair is the Lichtenstein tension-free mesh repair which places the mesh anteriorly between the external and internal oblique aponeuroses[8]. Other open mesh techniques include the plug-and-patch, the Gilbert Prolene Hernia System (PHS) Bilayer connected device repair, and the open preperitoneal mesh placed via an inguinal incision after reduction of the hernia[9,10]. The Stoppa repair, is an open preperitoneal mesh repair utilized for large inguinoscrotal and bilateral inguinal hernias, utilizing a lower midline incision[11]. The anatomic exposure of the Stoppa repair is the precursor for laparoscopic preperitoneal repairs. These aforementioned open surgical techniques allow for repair both with and without mesh, as well as placing mesh in various locations.
Classification of open and laparoscopic techniques for inguinal hernia repair
| Open | Laparoscopic | ||
| Mesh-free tissue repair | Bassini Marcy McVay Shouldice Desarda | ||
| Mesh repair | Anterior mesh | Lichtenstein Plug-and-patch Bilayer device (PHS) | |
| Preperitoneal mesh | Open preperitoneal via inguinal incision Stoppa | TEP TAPP | |
By utilizing the preperitoneal space and exposure of the myopectineal orifice described by Rene Stoppa, laparoscopic approaches to inguinal hernia repairs are a minimally invasive option to inguinal hernia repair by placing mesh in the preperitoneal space. There are two main methods of laparoscopic inguinal hernia repair with the same exposure and coverage of the myopectineal orifice but differences in how access to the preperitoneal space is gained. One approach avoids violation of the abdominal cavity (Totally Extraperitoneal - TEP repair) and one enters the abdominal cavity (Transabdominal Preperitoneal - TAPP repair). For both the TEP and TAPP repairs, dissection should ensure the critical view of the myopectineal orifice which routinely exposes the inguinal anatomy allowing any direct, femoral, obturator, or indirect hernias to be identified and reduced[12]. Although these laparoscopic methods necessitate mesh use, recent minimally invasive techniques utilizing robotic platforms may provide a means of mesh-free preperitoneal repair in selected patients with direct and/or indirect defects[13].
In the TEP repair, surgery is contained within the extraperitoneal space. This can provide an advantage when patients have had prior abdominal surgeries with the potential of adhesions and scar tissue complicating the procedure, but still allowing for a minimally invasive approach. In the TAPP repair, surgery takes place from the intraabdominal space and subsequent access to the preperitoneal space is gained by incising the peritoneum and creating a peritoneal flap. The transabdominal view allows for a deliberate evaluation of intraabdominal contents, such as when there is concern for ischemic bowel. Unlike the TEP repair which is able to use insufflation between the abdominal wall and the peritoneum, the TAPP repair requires the surgeon to actively retract the peritoneum during dissection. When considering laparoscopic repair, surgeon experience and skill allow for replicability, decreased surgeon experienced difficulty, and reduction of complications - large trocar sites should be properly closed to reduce the risk of a subsequent trocar site hernia, the extraperitoneal space should carefully be created during a TEP repair to avoid tears and large holes which can complicate and hinder exposure, access to the abdominal cavity and pelvic exposure should be performed carefully to avoid enterotomies and/or injury to the peritoneum, and dissection of the hernia sac away from cord structures should be methodical to avoid damage to nearby structures and creation of peritoneal holes.
LAPAROSCOPIC VS. OPEN
The argument of which method is superior - open or laparoscopic - is often had by surgeons. With the wide array of techniques, patient factors, and surgeon factors, determining applicability of published results to one’s own practice can be quite difficult. Evaluating the type of open or laparoscopic procedures being assessed, the patients’ surgical histories, hernia size and patient comorbidities, and investigating surgeons’ expertise with each study all can be confounding variables that affect the results of a study and make meta-analyses quite difficult with such heterogeneous study methods. We would argue that it is beneficial for surgeons to have baseline familiarity of the multitude of surgical procedures, become proficient in both mesh and mesh-free techniques as well as open and laparoscopic techniques to best tailor the surgery to the patient and the clinical circumstances, and follow personal outcomes to evaluate individual results.
Surgeon familiarity with technique and anatomy is of utmost necessity to ensure good outcomes and avoid complications. Gaining expertise with the Shouldice technique’s four layers is benefited by surgical repetition, as shown by the results from the study by Malik et al.[14], which demonstrated repair at the high volume Shouldice Hospital was far superior to those from lower volume hospitals (1.15% vs. 5.21%). Although the 2012 Cochrane review found the Shouldice repair to be the best of all open mesh-free techniques, it took longer, required a longer hospital stay, and still had higher recurrence rates compared with mesh repair[15]. Whereas only 36 Lichtenstein procedures were needed to gain proficiency with inguinal hernia repair[16], it has been shown that as many as 250 laparoscopic hernia procedures are needed to attain sufficient experience to ensure similar complication rates relative to open repairs[17,18]. Repetition of procedures increases competency, and exposure to nuanced differences, and, in turn, improves surgical skill and results.
Both the European Hernia Society (EHS) guidelines and the international guidelines for groin hernia management published by the HerniaSurge group in 2018, recommend open Lichtenstein and laparoscopic inguinal hernia repairs for nonrecurrent, unilateral inguinal hernias[19,20]. Based on surgeon experience, open and laparoscopic repairs are acceptable methods. However, there are specific clinical scenarios in which certain procedures may be more advantageous than others such as contaminated or infected wounds, recurrent groin hernias, patients with contraindications to laparoscopy, and scenarios where multiple groin hernias are suspected.
CONTAMINATED OR INFECTED WOUND
For emergent or urgent cases in which there is gross contamination with pus or stool, a mesh free repair is necessary. Because laparoscopic inguinal hernia repair necessitates mesh use while open inguinal hernia repair can be performed both with and without mesh, an open tissue repair is the technique of choice for inguinal hernias in the setting of infection or stool spillage. Although biologic and absorbable synthetic meshes have been used in these settings, it should be cautioned that these meshes are not FDA approved for use in an infected field[21]. For emergent or urgent cases with strangulated bowel requiring resection, where contamination is negligible, mesh use has been shown in small cohort studies to have acceptable surgical site infection rates[22,23]. For contaminated settings, the senior author often prefers to utilize the Bassini or McVay tissue repair technique after wound irrigation and/or bowel resection. In cases of incarceration with possible strangulation, diagnostic laparoscopy with placement of ports for a TAPP repair is utilized to allow for intraabdominal evaluation of bowel. If viable, a TAPP repair is performed with a macroporous polypropylene mesh. If not viable, bowel resection is performed, and an open Lichtenstein repair is performed if contamination is well controlled; otherwise, a Bassini or McVay tissue repair is performed.
RECURRENT INGUINAL HERNIA
In recurrent hernia cases, the operating surgeon benefits from knowing the manner of the prior repair and utilizing the non-violated plane. Where the prior repair was performed using an open approach with anterior mesh, a laparoscopic technique is the recommended course[20]. Where the prior repair was performed using a laparoscopic approach with preperitoneal mesh, an open approach with anterior mesh is recommended[20]. In patients with multiply recurrent groin hernias where both anterior and preperitoneal planes have been violated, subsequent repair methods should be based on surgeon expertise. For these difficult scenarios, the senior author first reviews all old operative notes and obtains recent pelvic imaging with a CT scan for evaluation of anatomy. Based on this information, a repeat open repair may be tried on patients with a hostile abdomen or operative notes demonstrating a previous difficult MPO dissection. Otherwise, a repeat preperitoneal approach is tried, usually with the utilization of the robotic platform, which the author finds to be helpful in both visualization and ease of retraction of the peritoneal flap.
CONTRAINDICATIONS (AND RELATIVE CONTRAINDICATIONS) TO LAPAROSCOPY
The ability to perform an open repair under local or regional anesthesia negates any risk that could arise with general anesthesia. The insufflation of laparosocpy requires general endotracheal anesthesia (GETA) and thus any patient population in which GETA is contraindicated cannot undergo laparoscopic inguinal hernia repair. The higher risk of intra-abdominal adhesions and scarred tissue planes of patients with prior pelvic and/or abdominal surgeries can make laparoscopic approaches more difficult and potentially increase morbidity. For these reasons, open repair is often the repair method of choice as it rarely violates the abdominal cavity or requires extensive pelvic dissection. However, there are published studies in the appropriately skilled and experienced surgeon’s hands, demonstrating that laparoscopic repair is safe and feasible in patients with prior pelvic and lower abdominal surgeries[24,25].
MORE THAN JUST A UNILATERAL INGUINAL HERNIA
The Stoppa repair is the only open repair that allows bilateral groin hernia repair through the same incision as a unilateral repair and does not require bilateral groin incisions. For patients with symptomatic bilateral inguinal hernias, laparoscopic repair allows repair for both the right and left sides through the same three small trocar incisions. Indeed, in our practice, all patients without contraindications to laparoscopy and with bilateral groin hernias are offered a minimally invasive approach for repair. For patients with suspected contralateral hernias, a TAPP repair is offered to allow for contralateral inspection during initial camera insertion. TEP repair can also be performed, but contralateral exploration requires dissection of tissue planes. In our practice, a thorough discussion is conducted with the patient preoperatively on the risks and benefits of concurrent repair of an asymptomatic contralateral hernia vs. waiting until symptoms develop to pursue repair. Based on patient preference, repair of the contralateral asymptomatic side may or may not be performed.
In reviews of both the Swedish and Danish hernia databases, femoral hernias were found in over 40% of surgeries for recurrent groin hernias in women[26,27]. The preperitoneal dissection and the evaluation of the myopectineal orifice in laparoscopic repair ensure any occult femoral hernias are evaluated and treated with the mesh covering the space. For this reason, the EHS and Herniasurge groups encourage laparoscopic groin hernia repairs in female patients, to reduce the risk of missed femoral hernias in open repairs where the floor is commonly not opened and explored[19,20]. In our practice, female patients with groin hernias are preferentially offered a laparoscopic or minimally invasive technique. If an open repair is performed, the femoral space is always explored, evaluated, and repaired if necessary, using a modified Lichtenstein technique.
COSTS OF REPAIR
Costs for inguinal hernia repair have been shown to be significantly lower for open inguinal hernia repair, with differences being attributable to operating time as well as disposable material costs. As with many cost calculations, results should be well scrutinized to determine applicability to a surgeon’s and patient’s specific circumstances, the items being included in cost estimates, and the time frame for which costs are evaluated. In the 2006 VA study evaluating overall healthcare costs over 2 years (including operative costs, subsequent inpatient and outpatient care, and medications), Hynes et al.[28] found laparoscopic repair was on average $638 more than open, though not statistically significant. Similarly, in the retrospective study by Spencer Netto et al.[29], open unilateral inguinal hernia repair was found to be significantly cheaper than laparoscopic repair (median total cost, $3207.15 vs. $3723.66; P < 0.001), while bilateral repair costs were almost similar (median total cost, $4574.02 vs. $4662.89; P = 0.827). In a prospective randomized control trial (RCT) by Feliu et al.[30], laparoscopic bilateral inguinal hernia repair was found to be faster, with shorter hospital stays, fewer recurrences, and lower postoperative complications than bilateral inguinal hernias repaired using the Lichtenstein technique. In a meta-analysis by Schmedt et al.[31], operative time for a unilateral open Lichtenstein repair was significantly shorter than laparoscopic repair (55.5 min vs. 65.7 min; P = 0.01)[27]. Due to variation in negotiated reimbursement rates, institutional cost evaluations by Jacobs and Morrison showed $731 higher income generation for an ambulatory surgery center with laparoscopic repair when compared to open, despite increased disposable costs of laparoscopic repair materials[32]. Although repair of unilateral groin hernia repair may be cheaper when performed open, it may net the performing institution more income when performed laparoscopically. It does appear that bilateral repairs performed laparoscopically are financially better. With the reduction of operative times and decreased costs of disposable materials, use of laparoscopy could become similar if not more financially reasonable for the repair of unilateral inguinal hernia repairs as well. By knowing personal operative times and hospital costs, surgeons can adjust their surgical techniques to make the most financially reasonable as well as clinically appropriate decision.
COMPLICATIONS
As previously stated, familiarity and expertise with a surgical technique are also reflected in surgical outcomes. Well conducted studies and published analyses provide varying results on laparoscopic and open inguinal hernia repair. In the 2004 RCT by Neumayer et al.[17] with the Veterans Affairs (VA) medical centers, comparing open mesh repair to laparoscopic mesh repair, the laparoscopic repair group had lower postoperative pain and quicker return to normal activities, but higher rates of complications and recurrences. These findings have been questioned, as the size of the mesh used for laparoscopic repair was not standardized and may have played a role in higher laparoscopic recurrences[33]. As well, the study included operating surgeons not sufficiently adept at laparoscopic repair (only 25 prior repairs were needed to qualify as a surgeon in the study) and posthoc analysis found significant differences in recurrence rates between surgeons who had performed fewer than 250 laparoscopic repairs vs. those who had performed greater than 250 repairs (> 10% recurrence vs. < 5% recurrence; P < 0.001)[17]. In the 2010 meta-analysis by Karthikesalingam et al.[34] of four RCTs comparing various open repairs to laparoscopic (TEP and TAPP) inguinal hernia repair, recurrence rates, chronic pain, hematoma formation, and need for additional operations were the same, while laparoscopic repair had less postoperative pain, fewer wound infections, faster recovery and return to work, but a longer operative time. In the 2005 meta-analysis by Schmedt et al.[31] comparing laparoscopic (TEP and TAPP) techniques to the Lichtenstein repair, laparoscopy had lower rates of wound infection, hematoma formation, nerve injury and chronic pain, and quicker return to work and daily activities, while open repair had fewer recurrences and seromas, and shorter operative times. In further analysis with removing the results from the 2004 Neumayer study, regarding the difference in recurrence rates of open and laparoscopic repairs, there was no statistically significant difference between laparoscopic and open repairs[17,29]. Consistently seen in these studies, laparoscopic repair appears to have quicker return to work as well as less postoperative pain.
WHEN TO UTILIZE EACH TECHNIQUE
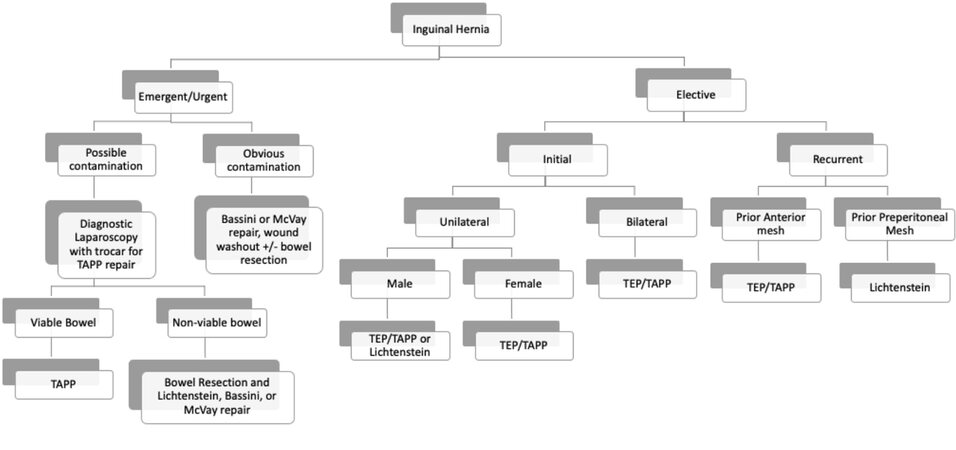
There are many variables to take into consideration, such as patient gender, type of groin hernia, wound class, whether it is unilateral or bilateral, and prior surgeries, when deciding on the method of repair. As well, a surgeon must take into account personal expertise with each surgical technique and determine the best type of repair for the clinical scenario. With that acknowledgement, in order to develop expertise, surgeons must progress through a learning curve and necessitate the need to accept longer operative times, higher costs when using adjunct disposables such as a dissecting balloon for TEP repair, and potentially higher incidences of complications such as seromas and hematomas. Once a surgeon feels competent with both laparoscopic and open techniques, an evaluation of personal outcomes should be made to determine what is the best method of repair to offer each patient. With equal expertise in open and laparoscopic repairs and evaluation of published data, patients with bilateral groin hernias, patients suspected of contralateral groin hernias, female patients with groin hernias, and patients with recurrent hernias after prior anterior mesh repair are offered minimally invasive and/or laparoscopic repair [Figure 1]. Patients with contraindications to general anesthesia or prior preperitoneal repair are offered an open Lichtenstein repair. Men with unilateral non-recurrent groin hernias or patients with histories of pelvic surgery and scarring are offered both open and minimally invasive/laparoscopic repairs, and differing risks and benefits are evaluated and weighed by the patient and surgeon to determine a mutually agreed upon method of repair.
Figure 1. Algorithm for inguinal hernia repair based on current literature. TEP: Totally extraperitoneal; TAPP: transabdominal preperitoneal.
There are many possible interventions when addressing inguinal hernias. There are variations of both open and laparoscopic techniques - from mesh to tissue repair and transabdominal to totally extra-peritoneal. Each surgeon must consider patient factors along with their own skill set and comfort level when deciding which technique to use. It is beneficial for surgeons to be well acquainted and facile with both open and laparoscopic techniques to provide a tailored approach to each patient. Like most things, the fact that there are multiple ways to perform a procedure is indicative that there may not be one truly best way. Equally important is that the surgeon becomes facile with the surgical technique, is knowledgeable of the anatomy and surgical principles of the operation, acknowledges the clinical situation, and follows the patients’ outcomes.
DECLARATIONS
Authors’ contributionsMade substantial contributions to literature review, manuscript writing, and editing: Burton V, Perez AJ
Availability of data and materialsNot applicabple.
Financial support and sponsorshipNone.
Conflicts of interestAll authors declared that there are no conflicts of interest.
Ethical approval and consent to participateNot applicabple.
Consent for publicationNot applicabple.
Copyright© The Author(s) 2021.
REFERENCES
1. Froylich D, Haskins IN, Aminian A, et al. Laparoscopic versus open inguinal hernia repair in patients with obesity: An American College of Surgeons NSQIP clinical outcomes analysis. Surg Endosc 2017;31:1305-10.
2. Bittner R, Arreguie ME, Bisgaard T, et al. Guidelines for laparoscopic (TAPP) and endoscopic (TEP) treatment of inguinal hernia [International Endohernia Society (IEHS)]. Surg Endosc 2011;25:2773-843.
3. Perez AJ, Strassle PD, Sadava EE, Gaber C, Schlottmann F. Nationwide analysis of inpatient laparoscopic versus open inguinal hernia repair. J Laparoendosc Adv Surg Tech A 2020;30:292-8.
4. Ramshaw B, Chiu S. Open Non-mesh Inguinal Hernia Repair. In: LaPinska MP, Blatnik JA, editors. Surgical Principles in Inguinal Hernia Repair A Comprehensive Guide to Anatomy and Operative Techniques. Cham: Springer International Publishing; 2018. pp. 33-8.
6. Shouldice EE. The treatment of hernia. Ontario Med Rev 1953;20:670-84.
8. Amid PK. Lichtenstein tension-free hernioplasty: its inception, evolution, and principles. Hernia 2004;8:1-7.
9. Rutkow IM, Robbins AW. "Tension-free" inguinal herniorrhaphy: a preliminary report on the "mesh plug" technique. Surgery 1993;114:3-8.
10. Gilbert AI, Graham MF, Voigt WJ. A bilayer patch device for inguinal hernia repair. Hernia 1999;3:161-6.
11. Stoppa R, Petit J, Abourachid H, et al. [Original procedure of groin hernia repair: interposition without fixation of Dacron tulle prosthesis by subperitoneal median approach]. Chirurgie 1973;99:119-23.
13. Huynh D, Fadaee N, Al-Aufey B, Capati I, Towfigh S. Robotic iliopubic tract (r-IPT) repair: technique and preliminary outcomes of a minimally invasive tissue repair for inguinal hernia. Hernia 2020;24:1041-7.
14. Malik A, Bell CM, Stukel TA, Urbach DR. Recurrence of inguinal hernias repaired in a large hernia surgical specialty hospital and general hospitals in Ontario, Canada. Can J Surg 2016;59:19-25.
15. Amato B, Moja L, Panico S, et al. Shouldice technique versus other open techniques for inguinal hernia repair. Cochrane Database Syst Rev 2012;2012:CD001543.
16. Paajanen H, Varjo R. Ten-year audit of Lichtenstein hernioplasty under local anaesthesia performed by surgical residents. BMC Surg 2010;10:24.
17. Neumayer L, Giobbie-Hurder A, Jonasson O, et al. Veterans Affairs Cooperative Studies Program 456 Investigators. Open mesh versus laparoscopic mesh repair of inguinal hernia. N Engl J Med 2004;350:1819-27.
18. Merola G, Cavallaro G, Iorio O, et al. Learning curve in open inguinal hernia repair: a quality improvement multicentre study about Lichtenstein technique. Hernia 2020;24:651-9.
19. Simons MP, Aufenacker T, Bay-Nielsen M, et al. European Hernia Society guidelines on the treatment of inguinalhernia in adult patients. Hernia 2009;13:343-403.
21. Köckerling F, Alam NN, Antoniou SA, et al. What is the evidence for the use of biologic or biosynthetic meshes in abdominal wall reconstruction? Hernia 2018;22:249-69.
22. Ueda J, Nomura T, Sasaki J, et al. Prosthetic repair of an incarcerated groin hernia with small intestinal resection. Surg Today 2012;42:359-62.
23. Atila K, Guler S, Inal A, Sokmen S, Karademir S, Bora S. Prosthetic repair of acutely incarcerated groin hernias: aprospective clinical observational cohort study. Langenbecks Arch Surg 2010;395:563-8.
24. Dulucq JL, Wintringer P, Mahajna A. Totally extraperitoneal (TEP) hernia repair after radical prostatectomy or previous lower abdominal surgery: is it safe? Surg Endosc 2006;20:473-6.
25. Callahan ZM, Donovan K, Su BS, et al. Laparoscopic inguinal hernia repair after prostatectomy: Evaluating safety, efficacy, and efficiency. Surgery 2019;166:607-14.
27. Koch A, Edwards A, Haapaniemi S, Nordin P, Kald A. Prospective evaluation of 6895 groin hernia repairs in women. Br J Surg 2005;92:1553-8.
28. Hynes DM, Stroupe KT, Luo P, et al. Cost effectiveness of laparoscopic versus open mesh hernia operation: results of a Department of Veterans Affairs randomized clinical trial. J Am Coll Surg 2006;203:447-57.
29. Spencer Netto F, Quereshy F, Camilotti BG, et al. Hospital costs associated with laparoscopic and open inguinal herniorrhaphy. JSLS 2014;18:e2014.00217.
30. Feliu X, Clavería R, Besora P, et al. Bilateral inguinal hernia repair: laparoscopic or open approach? Hernia 2011;15:15-8.
31. Schmedt CG, Sauerland S, Bittner R. Comparison of endoscopic procedures vs Lichtenstein and other open mesh techniques for inguinal hernia repair: a meta-analysis of randomized controlled trials. Surg Endosc 2005;19:188-99.
32. Jacobs VR, Morrison JE Jr. Comparison of institutional costs for laparoscopic preperitoneal inguinal hernia versus open repair and its reimbursement in an ambulatory surgery center. Surg Laparosc Endosc Percutan Tech 2008;18:70-4.
33. Strate T, Mann O, Izbicki JR. Open mesh versus laparoscopic mesh hernia repair. N Engl J Med 2004;351:1463-5.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Burton V, Perez AJ. Comparison of open and laparoscopic inguinal hernia repair. Mini-invasive Surg 2021;5:26. http://dx.doi.org/10.20517/2574-1225.2021.26
AMA Style
Burton V, Perez AJ. Comparison of open and laparoscopic inguinal hernia repair. Mini-invasive Surgery. 2021; 5: 26. http://dx.doi.org/10.20517/2574-1225.2021.26
Chicago/Turabian Style
Burton, Victoria, Arielle J. Perez. 2021. "Comparison of open and laparoscopic inguinal hernia repair" Mini-invasive Surgery. 5: 26. http://dx.doi.org/10.20517/2574-1225.2021.26
ACS Style
Burton, V.; Perez AJ. Comparison of open and laparoscopic inguinal hernia repair. Mini-invasive. Surg. 2021, 5, 26. http://dx.doi.org/10.20517/2574-1225.2021.26
About This Article
Special Issue
Copyright
Data & Comments
Data

 Cite This Article 135 clicks
Cite This Article 135 clicks










Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.